Research
Ongoing collaborative projects within BritPACT
Following the inaugural “Emerging Frontiers in PsA” meeting on 14th October 2015, a number of potential research and educational priorities were developed with the attendees of that meeting. Further survey work with the membership and steering committee has aimed to prioritise these unmet needs to inform the future collaborative projects in BritPACT.
Rheumatology editorial
Led by Dr Jon Packham, the steering committee published an editorial in Rheumatology outlining the role of BritPACT and the potential advantages to an independent network of PsA researchers in the UK who could lead on research and educational activities.
Support for MONITOR-PsA “Trials Within Cohorts”
Following an email to the BritPACT membership, five BritPACT members volunteered to support the Multicentre ObservatioNal Initiative in Treat to target Outcomes in Psoriatic Arthritis (MONITOR-PsA) study by serving as independent members of the Trial Steering Committee and Data Monitoring and Safety Committee. This study is running at the Universities of Oxford, Bath, Cambridge, Newcastle and Coventry and Warwick NHS Trust led by Dr Laura Coates.
Barriers to T2T qualitative research
Led by Dr Laura Coates (University of Oxford) and Dr Emma Dures (University of West of England), BritPACT have collaborated in a project to address the barriers and potential facilitators to implementation of a treat to target approach in PsA. This project ran through 2018 and 2019 and used qualitative research methods to explore the implementation gap in this field. In total, 10 BritPACT members took place in one-to-one interviews and 9 took part in a focus group held in March 2019. The study identified a number of potential barriers: an overarching theme of ‘Complexity’, which incorporated three themes of ‘PsA versus RA’, ‘Measurement’, and ‘Resources’. An underpinning theme of ‘Changes to current practice’ captured the tension between themes of ‘Reluctance due to organisational factors’ and ‘Individual determination to make changes.’ The data were presented at the American College of Rheumatology Annual Meeting in Atlanta in November 2019 and published in the Annals of the Rheumatic Disease in 2020 and available at https://ard.bmj.com/content/79/8/1031.long. Laura is now working an implementation RCT based on these findings.
Raising awareness of HQIP data
Analysis of the BSR HQIP audit data addressing outcomes in PsA was performed by Professor Neil McHugh and his team at Bath. Once this is published, BritPACT are aiming to raise awareness of this research highlighting the delay in diagnosis and impact of PsA in the UK.
Radiographic features of PsA
Dr Nicola Gullick and Professor Bruce Kirkham have proposed a project to investigate radiographic features of PsA in collaboration with a radiologist developing new analysis techniques. We hope to facilitate this research, identifying investigators and centres to participate and the ideas behind this project will be presented at the 2019 Annual Education and Training Day on Friday 22nd November 2019.
Education
Annual Education and Training Day on PsA
BritPACT have hosted an annual education and training day on psoriatic arthritis since the first in 2015. The attendance at these meetings has increased year on year with over 60 registered delegates.
Please go to our past meetings page for more information.
Our upcoming meetings can be found here.
Consensus-based Best Practice Statements
Starting in 2018 and led by Dr William Tillett, BritPACT will be developing consensus based best practice statements to help physicians integrate current national and international treatment recommendations with practical advice on optimising patient care. We aim to cover topics including screening, diagnosis, assessing prognosis, assessment of disease activity, management and comorbidities.
PSP
In 2019, a Psoriatic Arthritis Priority Setting Partnership (PSP) commenced aiming to identify unmet needs in psoriatic arthritis. This is being funded by Brit-PACT and led by Dr Laura Coates from the University of Oxford, in collaboration with the British Society of Rheumatology (BSR), Psoriasis Association and the Psoriasis and Psoriatic Arthritis Alliance (PAPAA).
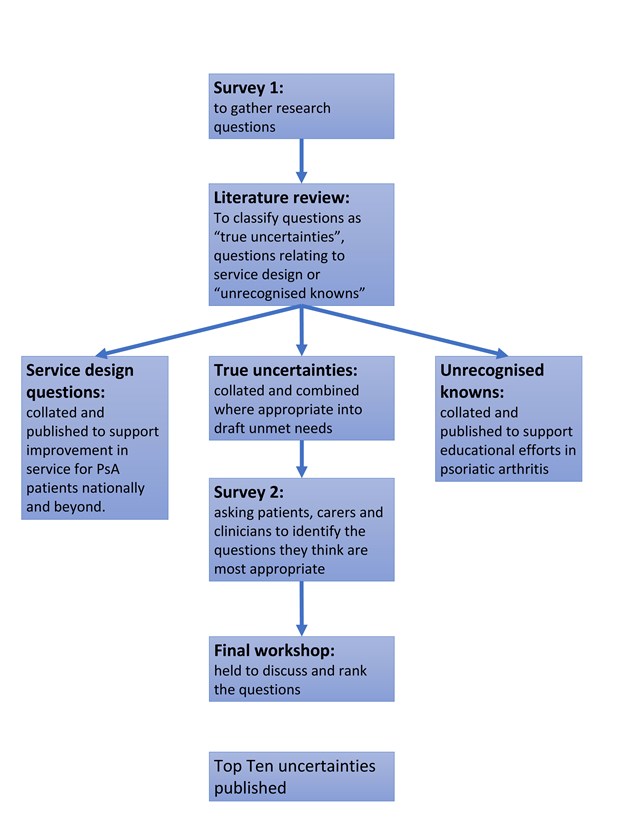
The project follows methods set out by the James Lind Alliance and have been used for many different conditions. The first step was to ask everyone affected by psoriatic arthritis – individuals who live with the condition, their families and friends and the clinicians who treat them what they perceive to be the unmet needs in psoriatic arthritis via a large online survey launched in June 2020. We asked them to submit key research questions that they want to see addressed. Over 300 people responded and almost 1000 questions were submitted. Once the survey closed in September, the responses were collated and grouped into eight themes, before being narrowed down into 46 summary questions related to psoriatic arthritis. The steering committee will check to ensure that these questions have not already been satisfactorily addressed by research studies. Any questions that are found to have already been answered by existing research studies, will be collected to share with healthcare professionals and research organisations so that they can think about how to better communicate this information to healthcare professionals and the public.
Then a second (shortlisting) survey was performed, again with all people affected by psoriatic arthritis invited to take part. The respondents were be asked to pick their top questions that matter to them most up to a maximum of ten questions.
After the results of the second survey were available, people with psoriatic arthritis, their families, and healthcare professionals were invited to a final workshop to discuss and rank the most popular questions from the survey, producing a final 'Top Ten' list. This list of priorities will help to inform researchers and research funders working in psoriatic arthritis, so that, in future, work is done in areas that are deemed most important.
Click to download the terms of reference and the protocol.
Top Ten Psoriatic Arthritis Research Priorities Announced
The 'Top Ten' list, agreed upon by patients, carers and clinicians, for the Psoriatic Arthritis Priority Setting Partnership (PSP)
Image of psoriatic arthritis PSP steering group
We are delighted to reveal the Top Ten Psoriatic Arthritis Research Priorities, agreed upon by people living with psoriatic arthritis, carers and healthcare professionals. This 'Top Ten' list was reached by agreement in a final prioritisation workshop. Research funders will consider the Top Ten list when planning future psoriatic arthritis research. They will use these questions to focus on areas that matter most to the people in the UK living with the condition and those involved in its care and treatment.
The project followed the James Lind Alliance's Priority Setting Partnership method. It began with an open call for psoriatic arthritis stakeholders to submit the questions they wanted to answer about the condition and its treatments. Nearly one thousand questions were received from people living with the condition, their families, GPs, Rheumatologists, Allied Health Professionals, Nurses and others. These questions were refined through a rigorous and collaborative process, including the second round of voting and a final workshop day to agree on the 'Top Ten'.
The Top Ten Psoriatic Arthritis Research Priorities are:
- What is the best strategy for managing patients with psoriatic arthritis, including non-drug and drug treatments?
- What factors affect how psoriatic arthritis will progress, the likely severity of the disease in an individual and whether it will go into remission?
- Can tests be developed to predict whether a person has or will develop psoriatic arthritis?
- Is a person with psoriatic arthritis at risk of developing other health conditions? If so, which ones? Why?
- Does treating psoriatic arthritis early (or proactively) reduce the severity of the disease and/or make it more likely to go into remission?
- What triggers acute exacerbations and flares of psoriatic arthritis symptoms?
- What is the best way to measure outcomes of treatment in psoriatic arthritis?
- What are the long-term risks and benefits of medications used for psoriatic arthritis?
- Why do treatments stop working well against psoriatic arthritis, and when they lose effectiveness, what's the best way to regain control of psoriatic arthritis?
- What treatments present the most benefit (considering efficacy, tolerability and safety) for the different body tissues involved in psoriatic arthritis, for example, joints, tendons, spine, skin and nails?
Professor Laura Coates, Lead for psoriatic arthritis PSP and Brit-PACT chair, comments, "Like all James Lind PSPs, this process in PsA was led by a strong steering committee representing both people with PsA and health-care professionals in the field. The input of so many people living with PsA, their families, and a wide variety of health care professionals has allowed us to identify key unmet needs in PsA and prioritise them to support future research. We are indebted to all of our partners but particularly the James Lind Alliance, British Society of Rheumatology (BSR), Psoriasis and Psoriatic Arthritis Alliance (PAPAA) and Psoriasis Association who offered substantial support throughout the process. We hope that this Top 10 will guide future research in the field to maximise benefit for people with the condition."
James Lind Alliance
The James Lind Alliance (JLA) is a non-profit-making initiative, established in 2004. It brings patients, carers and clinicians together in Priority Setting Partnerships (PSPs), the aim of which is to identify and prioritise uncertainties, or ‘unanswered questions’, about the effects of treatments and interventions in different health conditions, topics or settings.
The JLA believes that addressing uncertainties about the effects of treatments or interventions should become accepted as a much more routine part of clinical practice, and patients, carers and clinicians should work together to agree which, among those uncertainties, matter most and thus deserve priority attention.
The JLA is funded by the National Institute for Health Research (NIHR) and is coordinated through the NIHR Evaluation, Trials and Studies Coordinating Centre (NETSCC). To find out more about current and past PSPs, please visit www.jla.nihr.ac.uk.
PSP Committee
- Suzannah Kinsella, James Lind Association Advisor, James Lind Association
- Laura Coates, Rheumatologist, University of Oxford
- Louise Hailey, Research Assistant and Information Specialist, University of Oxford
- Jon Packham, Rheumatologist and BSR representative
- Philip Helliwell, Rheumatologist, University of Leeds
- Sandeep Mukherjee, Rheumatologist, Bournemouth and Christchurch NHS Hospitals Trust
- Helen Burstow, Rheumatology Specialist Nurse, Bournemouth and Christchurch NHS Hospitals Trust
- Christine Bundy, Psychologist, University of Cardiff
- Helen Young, Dermatologist, University of Manchester
- Elspeth Wise, General Practitioner
- Helen McAteer, Psoriasis Association representative
- David Chandler, Psoriasis and Psoriatic Arthritis Alliance representative
- Russ Cowper, Patient representative
- Lucille Joannes, Patient representative
- Bronagh Kennedy, Patient representative
- Andy Kelly, Patient representative
PSP partners
We are delighted that the following organisations support and have agreed to help promote the Psoriasis PSP to their networks:
- British PsA Consortium (Brit-PACT) – also funders
- British Society for Rheumatology (BSR)
- Psoriasis Association
- British Association of Dermatologists (BAD)
- Psoriasis and Psoriatic Arthritis Alliance (PAPAA)
- Bath Institute for Rheumatic Diseases (BIRD)
- Royal College of Nursing (RCN)
- Musculoskeletal Association of Chartered Physiotherapists (MACP)
- Primary Care Rheumatology and Musculoskeletal Medicine
- Podiatry Rheumatic Care Association (PRCA)
- Arthritis and Musculoskeletal Alliance (ARMA)
- National Rheumatoid Arthritis Society (NRAS)
- National Axial Spondyloarthritis Society (NASS)
- Arthur’s Place
- Barbara Ansell National Network for Adolescent Rheumatology (BANNAR)
- Bath Institute for Rheumatic Diseases
- College of Podiatry
- Juvenile Idiopathic Arthritis TSG
- Bath GP Education Research Trust
